Medical Negligence Solicitors
Trust Our Solicitors for Your Medical Negligence Claim
Our medical negligence solicitors provide legal support that you can trust. If you have been injured due to a medical accident, our lawyers can help get your life back on track. We offer no win no fee agreements, meaning there’s no financial risk to you in bringing a claim.
“Small but very effective and experienced team so every client benefits from the personal touch but also highly skilled litigation know-how. Capability of the team means they can handle all aspects of very complex cases as well as straightforward matters.”
“Osbornes Law is an established firm which handles a breadth of complex and high-value clinical negligence matters.”
We all expect the highest level of care from our healthcare professionals. Sadly, mistakes do happen that cause harm to patients. Sometimes, medical treatment is so poor that it may be deemed negligent. If you have suffered an injury or illness due to medical negligence, you may be entitled to compensation. Our medical negligence solicitors have the specialist expertise required to guide you through the process of making a claim.
Medical negligence is where an injury is caused, or an existing condition is made worse due to poor care provided by medical professionals. These include injuries that occur while being cared for by the NHS or private healthcare providers. The terms medical negligence and clinical negligence mean the same thing. We usually use the terms interchangeably.
Table of Contents
What is considered medical negligence?
Medical negligence is where an injury is caused, or an existing condition is made worse due to poor care provided by medical professionals. These include injuries that occur while being cared for by the NHS or private healthcare providers. The terms medical negligence and clinical negligence mean the same thing. We usually use the terms interchangeably.
What types of medical negligence can I claim for?
- Medical misdiagnosis – where a condition gets missed and goes undiagnosed or when a diagnosis is wrong, including misdiagnosis of cancer .
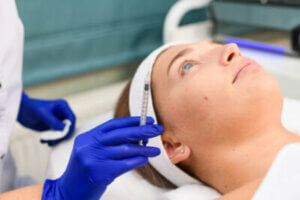
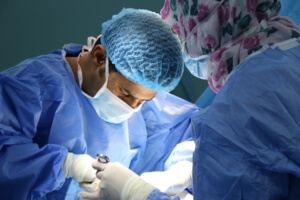
- Mistakes during surgery – include incidents where the wrong operation was performed, infections caused by poor hygiene and cosmetic surgery that has led to disfigurement or scarring.
- Prescription errors – you have been prescribed the wrong medication, incorrect dosage or together with another drug that shouldn’t be taken together.
- Negligent clinical advice – failure to warn of risks, including making alternative treatments clear so that you could make an informed decision.
- Pregnancy and birth injuries – sustained by the mother or baby during pregnancy, labour or after birth.
What types of medical professionals can be held liable for negligence?
Various medical professionals can be liable for negligence if they fail to meet the expected standard of care, causing harm to a patient. These professionals can include:
- General practitioners (GPs ), specialists, surgeons, and hospital doctors can all be held accountable for medical negligence.
- Nurses, nurse practitioners, and other nursing staff members may be liable if they breach their duty of care to a patient.
- Dentists and orthodontists can be liable for negligence if they provide substandard care or make mistakes during dental procedures.
- Pharmacists who dispense medication incorrectly or provide incorrect information about medications.
- Midwives can be sued for negligence if they fail to provide appropriate care before, during, or after childbirth, leading to harm to the mother or baby.
- Anesthesiologists who administer anaesthesia incorrectly or fail to monitor a patient’s vital signs during surgery.
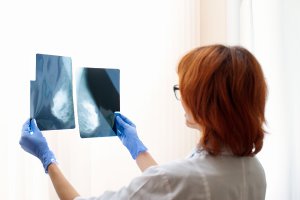
- Radiologists who misinterpret medical imaging, such as X-rays or MRIs, and provide inaccurate diagnoses
- Ophthalmologists (eye care professionals) if they provide incorrect prescriptions, misdiagnose eye conditions, or perform eye surgery incorrectly.
To establish a claim, it must be proven that the medical professional breached their duty of care and this breach directly resulted in harm or injury to the patient.
How do I know if I have a valid medical negligence claim?
Before taking on a medical negligence case, our solicitors will check that you have a valid claim. We will need to establish that:
- You were owed a duty of care by the healthcare provider. This duty is usually automatically established when a doctor-patient relationship exists.
- The clinician breached their duty of care. This typically involves demonstrating that their actions or omissions fell below the standard of care expected from a reasonable and competent healthcare professional. Sometimes, this is obvious, for example, if an instrument is left inside you after surgery, but more often it requires extensive medical evidence.
- The medical professional’s negligence directly caused your injury or worsened your condition. This is known as ‘causation.’ For example, imagine if a patient visits their GP several times with signs of cancer but the GP doesn’t refer them for tests. The GP’s actions may be negligent, but proving causation is more complex. It requires expert evidence to show that if the referral had been made earlier, treatment could have started sooner and that would have led to a better outcome.
- You suffered actual harm, injury, or financial loss due to the negligence. This can include physical injury, emotional distress, medical expenses, loss of income, or other damages.
The incident happened within the past three years or you became aware of the negligence no more than three years ago. There are a few exceptions to this rule but, generally, claims made after three years are considered time-barred and will not be accepted by the court.
How do I make a medical negligence claim?
Medical negligence claims can be complex and challenging, so it is vital to consult with a specialist clinical negligence solicitor to guide you through the process effectively.
Contact our specialist medical negligence lawyers
We’ll meet you face-to-face before taking the case on. The appointment can take place at your home, in a hospital or at our offices, whatever is best for you. We will assess your case and advise whether you have a valid injury claim.
Decide to work with us
Following our meeting, we’ll advise you about the prospects of success, the potential value of your medical negligence claim, and how long it will take. If we all agree that Osborne Law should take your medical negligence case on, we will discuss the funding of your claim, including whether to run your claim under a No Win No Fee agreement.
Throughout your case, you’ll have direct access to a dedicated case worker. They will keep you informed of the progress of your claim and consult you about all decisions relating to your case.
Investigate the claim
To help us prepare your claim, we’ll obtain a full set of your medical records and review them in detail. We will also take a detailed record of your version of events and check this against your medical records. Sometimes, there are discrepancies between your account and the medical records, which we need to know about when preparing your case.
Independent medical reports
To help prove that medical negligence occurred, we may consult an independent medical professional who specialises in a relevant field, for example, an oncologist or an orthopaedic surgeon. They will carry out a physical examination and prepare a medical report giving their opinion about your injuries, what treatment should (or should not) have been given, and how long it will take you to recover from your injuries.
The medical report helps us to establish a link between the substandard medical care you received and your subsequent health issues. It’s important that the medical assessment fully reflects your injuries so we can negotiate the settlement figure you deserve.
Letter of claim
We’ll write to the healthcare provider that treated you telling them that you’re taking legal action – this could be your GP or the local NHS Trust. While the Letter of Claim is not an official court document, it sets out your allegations and requests compensation. The healthcare provider has 14 days to acknowledge receipt of the letter and four months to conduct their own investigations and respond. At this point, we find out if the healthcare provider admits liability or disputes the claim.
Negotiate a settlement
If the healthcare provider accepts liability, we can start negotiating a settlement, based on what we think you’re entitled to. The amount will reflect the type and severity of your injuries, the impact they have on your quality of life, and financial losses such as loss of earnings, medical bills, and the cost of any future care you may need. We can also apply for an Interim Payment if you need urgent funds or medical care before the settlement is agreed.
Issue court proceedings
If the healthcare provider denies liability or we can’t agree a suitable settlement, we may need to start court proceedings. As a first step, the Court will set a timetable for the various stages of the litigation. This can stretch over many months so we keep negotiating with the other side and try to reach an agreement before a court hearing is necessary. We may arrange mediation or some form of alternative dispute resolution at any point of the claim, as this can often lead to a faster, more amicable outcome and help keep costs down.
Settlement or court decision
Only a very small percentage of medical negligence claims go to trial. If yours does, then a judge will decide on the outcome after hearing evidence from both sides. You will receive compensation for your injuries, financial losses and legal costs if successful. If unsuccessful, you may not receive compensation and may have to pay the defendant’s legal costs.
How long do I have to file a medical negligence claim?
Medical negligence claims are subject to strict time limits, which, if missed, means you could lose the opportunity to pursue your case forever. This time limit is known as the limitation period.
We recommend against judging the calculation of your limitation period without expert advice from a specialist solicitor.
The law governing the medical negligence limitation period is set out in The Limitation Act 1980. In short, you must issue a Claim Form at Court within three years of the date of negligence or the date you first knew about the negligence, whichever is later.
Calculating the limitation period is fraught with complications, so it is important to take legal advice as soon as possible to bring a claim. There are particularly complex rules for assessing the “date of knowledge” of the negligence.
The three years can slip by quickly, and delay increases the risk of losing vital evidence. Therefore, we recommend consulting a solicitor, ideally no later than 12-18 months after the incident of negligence, to avoid the problems caused by delay and to give your claim the best chance of success.
Are there any exceptions to the medical negligence limitation period?
- Suppose someone has died due to medical negligence. In that case, the limitation period is calculated to expire three years from the injured person’s death date or the date of the Personal Representative’s knowledge, whichever is the latter.
- The limitation period for any claim brought by a child (defined as those under the age of 18) does not begin to run until the date of their 18th birthday, which effectively means that they have until their 21st birthday to issue court proceedings.
- Where the person bringing the claim lacks mental capacity, there is no time limit for issuing court proceedings. Assessing capacity is not always straightforward, and solicitors must tread carefully when determining whether their client lacks the capacity to make their own decisions.
- The Court has the power to exercise its discretion to allow court proceedings to be issued outside of the limitation period, but this is reserved for exceptional cases, and there are very specific criteria set by the courts to trigger the Court’s discretion to allow a claim to proceed out of time.
How long do medical negligence claims take?
It is very difficult to say exactly how long a medical negligence claim will take from start to finish. It depends on the nature of your case, the complexity of your case, and how long it takes to obtain all the evidence (medical records, witness statements, medical reports, etc).
It also depends on the stance the Defendant takes. The NHS Trusts will usually report to the NHSLA, the governing body of the NHS Trusts. A lot will depend on the attitude of the NHSLA and/or the Trust.
If legal proceedings are needed, they must be issued at Court no later than 3 years after the date of your injury or 3 years from the date that you knew that the treatment/care you received was negligent. This may happen at a later date, i.e. when you are seen by another specialist, who then diagnoses your injury, explains the cause of the injury to you and explains that it was related to previous medical care that you received.
We can provide advice on any tertiary advice and assistance that you may require during the life of your claim. If the Defendant admits liability for your injury, we can apply for an interim payment of damages on your behalf to assist in speeding up the litigation process.
How much compensation will I receive when making a medical negligence claim?
Compensation amounts for medical negligence claims can vary significantly based on individual circumstances. Several factors are considered to determine the amount. These include the severity and impact of the injury, loss of earnings, future care needs, and any additional expenses incurred due to the negligence. Read our guide to NHS compensation payouts.
Here are some examples of compensation that our clients have received:
- Spinal Fracture Case Settles for 6-figure Sum
- 5-figure settlement for infusion leak to mother
- Perineal Tear case settles for 6-figure sum
- Six-figure claim allows family to move home
- Likely settlement of £15-20 million
Our Medical Negligence Case Studies provide further examples of successful compensation claims.
Experienced medical negligence solicitors
Osbornes Law has been helping individuals and families for nearly 50 years. Our medical negligence lawyers are accredited by and are members of the leading charity campaigning for patient safety and justice, Action against Medical Accidents (AvMA). We hold Law Society Clinical Negligence Accreditation, and the Solicitors Regulation Authority (SRA) regulates our solicitors.
Our dedicated team has extensive experience in supporting families with medical negligence claims. This expertise is complemented by a deep understanding of medical terminology and procedures, allowing us to identify irregularities in clients’ medical records effectively.
Our medical negligence services
Our lawyers have helped clients pursue a wide range of medical negligence claims, including the following:
- Birth Injury Claims
- Cancer misdiagnosis
- Brain Injuries
- Spinal Cord Injury
- Fatal medical negligence claims
- Cardiac claims
- Cauda Equina Syndrome Claims
- Care Home Claims & Nursing Home Claims
- GP Negligence Claims
- Infectious Disease Claims
- Ophthalmology Claims
- Orthopaedic Claims
- Pressure Sore Claims
- Pulmonary Embolism Claims
- Surgical Negligence Claims
- Vaginal Mesh Claims
If you have been affected due to poor medical treatment, contact our London solicitors today, and we will help establish whether you may bring a claim.
Do I need medical negligence solicitors near me?
No, we advise clients throughout the UK regarding making medical negligence claims. Take a look at our client stories to understand the type of successful claims we have made.
The team at Osbornes are medical negligence claims specialists, as evidenced by their accreditation from the leading clinical negligence panels. We’ve been fighting our clients’ corner for over 50 years and have a track record of securing multi-million-pound settlements for clients whose lives have been devastated by the most serious injuries due to substandard medical care.
Our promise to you:
- We only represent the injured party, not healthcare providers, so there’s never a conflict of interest
- We provide a free initial consultation and case review with no obligation to make a claim
- We will help you navigate the challenging NHS complaints procedure so you get the answers you need – as well as the compensation you deserve
We know you will have questions before deciding to begin a claim. Please call or visit us in our Camden or Hampstead offices for a free, no-obligation consultation; we’ll gladly help you.
No win no fee medical negligence claims
Your no win no fee medical negligence claim may be funded by:-
- Conditional Fee Agreements ( No Win No Fee agreements )
- Before the Event Insurance (BTE)
We offer a Conditional Fee Agreement (No Win No Fee Agreement), and we can offer delegated After the Event (ATE) insurance with deferred premium (payable at the end of the case) to protect you against any adverse costs.
We use the Law Society’s approved Conditional Fee Agreement.
Our guarantee
We guarantee that you will not have to pay anything if we are unsuccessful in obtaining compensation for you. If this happens, we are paid nothing.
If your claim is successful, you may have to pay legal fees and expenses out of your compensation, but we guarantee that this will not exceed 25% of the compensation awarded to you and this includes the ATE insurance premium and IPT.
These guarantees only apply if you pursue your claim with us for as long as it has reasonable prospects of success, follow our professional advice and do not deliberately mislead us.
The deduction from damages
There are two elements to the deduction from damages:-
- A “success fee” to cover us for the risk of losing your case and being paid nothing.
- A premium for insurance to cover you against the risk of having to pay the other side’s legal fees or your expert fees and expenses.
We guarantee that the deductions will not exceed a maximum of one-quarter of your compensation.
The success fee is a percentage uplift on our normal fees to cover us for the cases we lose. It is not a percentage of your compensation.
The amount of the success fee depends on how risky your case is. The riskier, the higher the percentage uplift on our normal fees.
ATE Insurance cover
The insurance policy is to cover you against two risks:-
- We will fund the experts’ fees and other expenses. If your claim succeeds, the other side will pay these expenses. If it is unsuccessful, the insurance company pays these fees for you.
- If you reject a formal offer of settlement and then a Judge awards you the same amount or less, the normal rule is to pay the other side’s costs from the date you should have accepted the offer. However, if we advised you to reject the offer and you took our advice, the insurance will pay the other side’s costs.
Remember that we guarantee that the success fee and the insurance premium combined will not exceed 25% of the compensation awarded to you.
If you have BTE insurance cover that provides cover for you for clinical/medical claims at the time of your injury. In that case, we can write to your insurers to request coverage under such a policy to investigate your potential claim.
Medical Negligence FAQS
Will I have to go to court to settle my medical negligence claim?
It is rare for medical negligence claims to go to court. Most cases are settled once all the investigations are completed before legal proceedings are issued.
Where proceedings are issued, as long as the case has good supporting medical evidence, most cases settle without the need to go to court.
It is in everyone’s interest to avoid court, so both sides are encouraged to settle matters quickly to avoid extra costs.
However, even though most cases settle well before going to trial, you should ultimately be prepared for going to court so a judge, having heard all the evidence, can decide whether the treatment was negligent.
What is a patient recall letter?
A patient recall letter is sent by a hospital or healthcare provider to people who previously have received treatment from them. The letter explains that there may have been an issue with the treatment received or the actions of an individual medical professional and asks the recipient to come in again to be re-examined.
What is a Letter of Claim?
A letter of claim is a formal document that our lawyers send to a healthcare provider, alleging that negligent care caused harm. This letter outlines the details of the negligence, the resulting injuries, and the compensation sought. It is the first step in the pre-action protocol for medical negligence claims, aiming to inform the healthcare provider of the claim and encourage early resolution without court proceedings.
What should I do if I get a patient recall letter from a hospital or health board?
The first thing is to attend the recall appointment and get checked out. Stay calm. Getting a patient recall letter may be concerning, but it doesn’t necessarily mean that you have been a victim of medical negligence. The hospital or healthcare provider is simply taking precautionary measures to ensure the safety and well-being of their patients.
If you have concerns about the medical treatment or diagnosis you received, speak to our medical negligence team. The patient recall letter serves as a record, acknowledging that the healthcare provider is aware of the potential claim. However, this does not mean that you should accept any offer of settlement from the healthcare provider without consulting with our team first, as it may not be a fair amount for your specific case. Our experienced solicitors can assess your situation and advise you on the best course of action to take.
Can I change solicitors if I'm not satisfied with my current solicitor?
Our team regularly receives calls from clients who have instructed other law firms, asking, “Can I change my solicitor?”
If you have a claim but are not happy with the advice you are receiving, we have specialist solicitors able to assist.
Speak to a specialist Medical Negligence Solicitor
Call us to speak with a lawyer 020 7485 8811
Email us Send us an email and we’ll get back to you
Medical Negligence Client StoriesVIEW ALL
- 10.7.2025
Osbornes Law Secures £700K in Crohn’s Negligence...
Negligent delay in diagnosing Crohn’s disease leads to £700K settlement Jodi Newton, Partner, was instructed in a case against...
Read more - 13.5.2025
Damages Recovered for Necrotic Pressure Sore
Elline Demetriou recovers damages following a necrotic pressure sore on her client’s heel Elline Demetriou, Solicitor in our clinical...
Read more - 6.5.2025
Six-Figure Settlement for Negligent C-Section Delivery
Osbornes secures a six-figure settlement following a negligent caesarean section delivery Jodi Newton, Partner and head of our Obstetric and...
Read more - 6.5.2025
Six-Figure Settlement for Negligent Shoulder Surgery
Settlement following a claim against Bedfordshire Hospitals NHS Foundation Trust Elline Demetriou, a Solicitor in our clinical negligence team, acted...
Read more - 29.4.2025
Five-Figure Settlement in Fatal Medical Negligence Case
Osbornes Law secures a five-figure compensation following a fatal medical negligence claim Osbornes acted for our client, E, who brought...
Read more - 4.2.2025
Claim Settled for Child’s Surgery Injuries
Osbornes secures settlement for child’s surgery-related injuries Osbornes Law successfully represented a minor, X, in a claim against two...
Read more - 29.1.2025
£27,000 DVT Claim Settled Against Royal Free London NHS
Successful settlement for DVT case against Royal Free London NHS Foundation Trust Successful Settlement of £27,000.00 for DVT Claim against Royal...
Read more - 14.10.2024
Multi-Million Settlement in Cerebral Palsy Negligence Case
Judge awards multi-million settlement in cerebral palsy medical negligence claim Jodi Newton, Partner and specialist medical negligence lawyer at Osbornes...
Read more - 12.9.2024
Great Ormond Street Hospital Negligence & How to Claim
Review of negligence at Great Ormond Street Hospital At Osbornes Law, we’ve supported families through some of the most...
Read more - 29.8.2024
AB v Central London Community Healthcare NHS Trust
Background Our client, AB, had been using the Nexplanon contraceptive device for 6 years. She had a Nexplanon device inserted into...
Read more - 17.7.2024
Settlement for Delay in Wrist Fracture Treatment
Our Clinical Negligence team have recently agreed the settlement of a case relating to a delay in the treatment of...
Read more - 28.6.2024
£55,000 Settlement for Stillbirth Claim Against Chelsea and Westminster...
Successful Settlement for Stillbirth Claim Against Chelsea and Westminster Hospital NHS Foundation Trust Background Nick Leahy, an Associate in our...
Read more - 9.5.2024
Claim Against Royal Free London NHS Foundation Trust...
Client obtains settlement after being victim of a surgical negligence Jodi Newton, Partner in our Clinical Negligence department, recently settled...
Read more - 30.4.2024
Settlement In Neonatal Death Case
Settlement in fatal medical negligence case against King’s College Hospital Nick Leahy, Associate in our Clinical Negligence department, recently...
Read more - 8.4.2024
Epilepsy Negligence Compensation Claim
Nicholas Leahy, an Associate in the Clinical Negligence team at Osbornes Law, has recently settled a long-running fatal medical negligence...
Read more - 5.1.2024
Delayed Pre-Eclampsia Diagnosis Results in Loss of Baby
Introduction to the case Nick Leahy, Associate in our Clinical Negligence department, has recently settled a birth injury claim against...
Read more - 23.11.2023
Claim against Bradford Teaching Hospitals NHS Foundation Trust
High-risk pregnancy following previous miscarriage Osbornes acted for a Claimant, C, in her birth negligence claim against Bradford Teaching Hospitals...
Read more - 21.9.2023
Large Compensation for Delayed Laryngeal Cancer Diagnosis
Actress receives financial award after life-changing missed cancer diagnosis. Jodi Newton acted for a client who was belatedly diagnosed with...
Read more - 21.9.2023
Delayed cervical cancer diagnosis client story
Introduction Jodi Newton acted for a woman who died following a delayed cervical cancer diagnosis. The deceased could have been...
Read more - 19.9.2023
Appendicitis Compensation Claim
Appendicitis misdiagnosis case settles for 5-figure sum Osbornes Law were instructed in a medical negligence claim against Bedfordshire Hospitals NHS...
Read more - 19.9.2023
Spinal Fracture Case Settles for 6-figure Sum
Spinal Fractures following cessation of Denosumab injection Case Overview Stephanie Prior was instructed in a spinal injury claim against Mid...
Read more - 13.9.2023
Delayed Basal Cell Carcinoma diagnosis client story
Settlement for delayed diagnosis of Basal Cell Carcinoma We are pleased to have successfully secured a settlement for our client...
Read more - 1.8.2023
Bowel Ischaemia Fatality – Client Story
Jodi Newton, a Partner in the Clinical Negligence Department at Osbornes Law, has recently settled a long running fatal medical...
Read more - 19.6.2023
Prison Healthcare Negligence
Nicholas Leahy, a solicitor in the Clinical Negligence Department at Osbornes Law, has recently successfully settled a long running case...
Read more
Osbornes are always professional and diligent in respect of their clients.
Osbornes has an excellent depth of experience across the team.
Across the board, they are all a pleasure to work with. They always keep a pragmatic head and all have an eye on the best outcome for the client.
Small but very effective and experienced team so every client benefits from the personal touch but also highly skilled litigation know-how. Capability of the team means they can handle all aspects of very complex cases as well as straightforward matters.
Osbornes is a very respected firm in the marketplace.
They handle really complex cases very well
The clinical negligence team are knowledgeable and professional in their approach and demonstrate a high level of skill in litigation work.
Osbornes Law offers experience in obstetric and fatal claims as well as niche cauda equina cases.
Osbornes Law is an established firm which handles a breadth of complex and high-value clinical negligence matters.
Osbornes has a skilled team of solicitors advising clients on a wide range of clinical negligence matters.
Hard working, approachable, good knowledge of clinical negligence and clients’ specific conditions
A joy to work with and always 100% client focused at all times.
The clinical negligence team at Osbornes is much lauded for its ability to ‘represent the diverse range of London-based clients
“The team is very quick and efficient in responding."
"Obsbornes Law is always client-focused and works tirelessly to obtain the best outcomes for clients."
They are an excellent firm who achieve fantastic outcomes for their clients. They are also very prominent in injuries to those travelling to or from Europe. Multiple languages are spoken by the team.
Stephanie Prior is a first-rate clinical negligence specialist whose industry, great experience and medical background put her in an exceptional class.
This firm is responsive and efficient. Their rapidity in dealing with complications or hiccups is excellent.
Really great clinical negligence practice, staffed by experienced practitioners who know how NHS Trusts work. They also build great rapport with clients.’
Stephanie has developed a particularly strong reputation for her handling of birth injury claims, as well as cases concerning surgical negligence and delays in surgery.
"An excellent firm which achieves fantastic outcomes for clients."
"Stephanie Prior takes on complex cases and gets excellent results. She has a background in medicine which serves her clients well and is a realistic but tough litigator."
"Stephanie Prior is hugely dedicated, adored by her clients, tenacious, efficient and extremely knowledgeable."
"Stephanie Prior is very good with troubled clients and is easily able to make them feel at ease."
"Stephanie shows sensitivity and deals with things in an understanding way."
Osbornes provides a very intimate and personal client service which is increasingly rare in this sector.
The lawyers in the team are highly experienced and will drive cases very hard on behalf of their clients.
"Stephanie Prior has a realistic attitude to the complexities of the cases. She wins the trust of her clients and goes the extra mile to ensure they get the best outcomes."
"Stephanie Prior... manages a varied caseload, including obstetric claims, child and adult brain injury cases and fatal and non-fatal spinal cord injury cases."
"Stephanie is experienced, knowledgeable of all aspects of clinical negligence work, and strategic in running cases."
"The team were extremely professional in putting my needs first. There was a joined-up approach to catering for the client, and all lawyers involved were briefed and constructive."
Stephanie Prior is always very professional and kind. Highly recommended.
Quite simply excellent, with a highly competent and well-rounded team. They understand complex medical litigation and have been our lifesavers, and we will always owe them our immense gratitude.
Essential Reading
Medical Negligence News & InsightsVIEW ALL
- 12.5.2025
Complaints Against Suspended Surgeon Ms Kuldeep Stohr
Ms Kuldeep Stohr, orthopaedic surgeon at Addenbrooke’s Hospital suspended In February 2025, Cambridge University Hospitals NHS Foundation Trust (CUH) confirmed...
Read more - 4.4.2025
Time To Move On From Physician Associates?
BMA raises concerns over patient safety: the risks of Physician and Anaesthesia Associates in the NHS The British Medical Association (...
Read more - 13.3.2025
Addenbrooke’s Hospital Complaints
Review finds harm to children by surgeon at Addenbrooke’s Hospital An independent review by Cambridge University Hospitals NHS Foundation...
Read more - 19.9.2024
Report highlights failings in maternity care
The Care Quality Commission (CQC) has recently carried out a national review of 131 maternity inspections between 2022 and 2024, finding that failures...
Read more - 30.7.2024
What Is the Role Of a Physician Associate?
What does the Position of Physician Associate Mean for the NHS? There are many different jobs within the NHS, each...
Read more - 11.1.2024
New UK Supreme Court Ruling regarding Secondary Victims...
The Supreme Court has today, on the 11th January 2024, upheld the Court of Appeal’s order to dismiss the claims...
Read more - 11.1.2024
Secondary Victim Claims
Secondary victims in clinical negligence cases What is a secondary victim in clinical negligence cases? Most compensation claims are concerned...
Read more - 12.12.2023
NHS Compensation Payouts Guide
What Are NHS Compensation Payouts? In the UK, the National Health Service delivers the vast majority of healthcare services. When...
Read more - 31.8.2023
Can you sue the NHS for waiting times?
The NHS is facing an unprecedented challenge with 7.47 million people waiting for routine treatments. This crisis impacts everyone, from those...
Read more - 31.8.2023
Hyponatraemia – Symptoms, Causes & Negligence
What is hyponatraemia? Hyponatraemia is a condition where sodium levels fall below a certain level, which can be dangerous. All...
Read more - 10.8.2023
Ambulance Delays Affecting Rapid Patient Treatment
Failure to Meet Ambulance Response Targets In 2017, the Secretary of State for Health accepted the new ambulance performance standards recommended...
Read more - 26.7.2023
Private Healthcare Negligence
Can you claim medical negligence against a private hospital? Yes – it can be a little more complicated than bringing a...
Read more - 9.6.2023
Early Notification Scheme – is it helping or failing...
What is the Early Notification Scheme? The NHS Early Notification Scheme (“ENS”) has reached its sixth anniversary. Established in April 2017,...
Read more - 23.3.2023
Private Pregnancy Scans and Substandard Care
In the news, it has been reported that private clinics that offer pregnancy scans to women are not meeting the...
Read more - 14.2.2023
The risk of extravasation injuries during iron infusion...
Many patients with low iron, particularly during pregnancy or postnatally, may be advised they need an iron infusion such as...
Read more - 9.11.2022
Delayed transfer to Accident & Emergency causing harm
The Healthcare Safety Investigation Branch (HSIB) has identified that patients may come at risk of harm whilst waiting in ambulances...
Read more - 9.11.2022
Breast cancer screening mammograms and negligence
Breast cancer screening has improved significantly in the UK due to research bettering the understanding of this terrible disease, which...
Read more - 21.9.2022
Are maternity services safe? – Part 2
In April last year I wrote a piece about government setting up a taskforce to look into why there are...
Read more - 8.9.2022
Poor interpretation of CTG can result in stillbirth...
Poor interpretation of a Cardiotocograph, more commonly known as a CTG, is a leading cause of stillbirth and brain injuries...
Read more - 14.7.2022
Insulin overdose in hospitals due to limited staff...
A century ago, insulin was first used to treat a 14-year-old boy dying of type 1 diabetes. A hundred years later,...
Read more - 6.7.2022
NHS aims to reduce waiting times with Elective...
The NHS recently recorded their waiting list to be at 6.5 million, a record high. Much of this backlog is due...
Read more - 29.6.2022
Nottingham Maternity: Donna Ockenden to Chair Independent Inquiry
An interim report on the state of maternity services at Nottingham University Hospitals NHS Trust has just been released. However,...
Read more - 23.2.2022
Women from ethnic minorities experience worse maternity care
It has been reported today that the government has set up a new task force to look into why there...
Read more - 13.1.2022
Secondary Victim Claims
Court of Appeal Judgement on Secondary Victim Claims Judgment was today handed down by the Court of Appeal in the...
Read more