Importance Of Timely Diagnosis In Heart Attack Cases
22 May 2019 | Stephanie Prior
Table of Contents
Every year in the United Kingdom there are over 200,000 hospital visits due to heart attacks, which equates to one visit every three minutes. However, since the 1960s there has been a significant improvement in survival rates, with seven out of ten patients now surviving after suffering a heart attack, primarily due to improved medical treatment for heart attack patients. Despite this improvement, the United Kingdom still has lower survival rates than other advanced economies. For example, a recent study published in the British medical journal The Lancet found that death rates for UK patients following a heart attack were 30 per cent higher than for Swedish patients (Sweden is a world leader in cardiac care).
Heart Attack
A heart attack happens when one of the coronary arteries, which provide blood to the heart muscle enabling it to function, becomes blocked. This prevents oxygen being supplied to the heart muscle, and the result is that the muscle will begin to die. There are two main types of heart attack, the most serious of which is known as an ST segment elevation myocardial infarction (or STEMI), in which the interruption to the blood supply to the heart muscle is caused by a total blockage of the coronary artery. The other is known as a non-ST segment elevation myocardial infarction (NSTEMI), in which the blood supply to the heart muscle is partially as opposed to totally blocked. However, without urgent treatment NSTEMI can progress to STEMI.
The most common symptoms of a heart attack include pain or discomfort in the patient’s chest, which occurs suddenly. This pain may spread into the left or right arm and also to the neck, jaw, stomach and back. It is also very common for patients to feel nauseas, sweaty and to be short of breath.
As these symptoms are most commonly experienced suddenly and when the patient is at home or in a non-hospital environment, it is important to call an ambulance as soon as possible.
Early Diagnosis and Treatment is Key
Diagnosis
In cases of acute myocardial infarction (AMIs), early diagnosis and urgent specialist treatment, followed by cardiac rehabilitation to reduce the probability of a recurrent heart attack or death, is essential. It is important to restore blood flow to the damaged heart muscle as soon as possible, and the restoration of this blood flow, in order to limit the amount of irreversible damage to the heart muscle, can be life-saving.
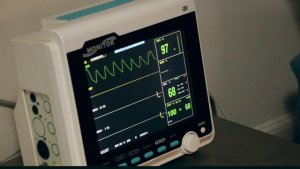
The most important diagnostic test for suspected heart attack patients is an electrocardiogram (ECG). An ECG test should be carried out within 10 minutes of the patient’s first medical contact, be that with an ambulance crew or at hospital, in accordance with NICE guidelines. The ECG test measures electrical activity within the heart and allows doctors to determine how well the heart is functioning. The ECG will help to determine the type of heart attack the patient has had, and therefore the most appropriate treatment path.
In addition, patients with suspected heart attack should have cardiac troponin measured in a peripheral blood sample taken at the time of their arrival to hospital, and should undergo serial troponin testing thereafter. Troponin is a protein which is released into the patient’s bloodstream during a heart attack and therefore elevated troponin levels help doctors diagnose a heart attack and provide the relevant treatment as early as possible.
Treatment
The treatment options are dependent on whether the patient has suffered STEMI or NSTEMI. STEMI is the most serious form of heart attack and so treatment should commence as soon as possible after diagnosis. If symptoms commenced within the past 12 hours, the patient will normally undergo primary percutaneous coronary intervention (known as PCI).
Patients presenting with STEMI will be rapidly transported by ambulance to a PPCI cardiac centre, and will thereafter be taken to a catheter lab for emergency PCI with stenting to open the acutely closed artery (revascularisation). This has the effect of preventing further damage to the heart muscle but is only of value within the first 12 hours of a heart attack (but for maximum benefit, within the first 6 hours).
For patients presenting with NSTEMI (or unstable angina), blood thinning medication including aspirin is usually recommended. Even in these cases, coronary angioplasty or coronary artery bypass graft may be recommended after initial treatment with the above medication.
Consequences of Delay
As is mentioned above, the treatment of heart attacks in the United Kingdom and the consequent survival rates have improved in recent years. However, sometimes things can go wrong and treatment can be delayed, with life-altering consequences for the patient concerned.
Osbornes Law have acted in many cases where there was a delay in diagnosis and treatment of a heart attack.
At Osbornes Law we care about how you are treated both by medical professionals at your GP surgery or at hospital and also under the care of private providers of health services. If you think that the care you or a loved one has received fell below the standard expected of a reasonably competent professional, then please do not hesitate to contact Partner and specialist medical negligence lawyer Stephanie Prior on 020 7681 8671.
Share this article
Contact
Client StoriesVIEW ALL
- 4.1.2022
Five-figure Compensation for Cardiac Negligence
In this cardiac negligence claim, we were instructed by a 42-year-old Polish man who had attended the Accident and Emergency...
Read more - 4.1.2022
6 Figure Settlement For Heart Attack Claim
In this cardiac claim, we were instructed by the widow of a 55-year-old man, who had complained of chest pain...
Read more - 13.7.2021
Family In Cardiac Negligence Claim Against NHS Trust
Nick Leahy, medical negligence solicitor at Osbornes Law was instructed to pursue a cardiac compensation claim on behalf of the...
Read more